
Matthew Trainer, chief executive of Barking Havering and Redbridge University Hospitals Trust, described this winter as the most challenging he can recall. The sheer volume of patients presenting at the trust’s two east London emergency departments—Queen’s Hospital in Romford and King George Hospital in Ilford—reached unprecedented levels in December, with nearly 1,000 individuals requiring treatment daily. This surge has exacerbated a persistent issue: "corridor care," where patients are treated on trolleys in hospital hallways due to a lack of available beds.
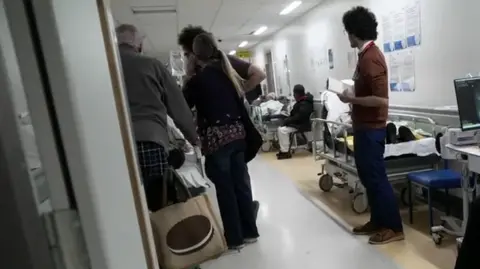
During a visit to Queen’s Hospital, the stark reality of this situation was evident, with 51 patients receiving care on trolleys lining the corridors of the emergency department. This marks the third consecutive winter where "corridor care" has become a necessary, albeit deeply concerning, operational strategy. While the hospital has attempted to mitigate the challenges by installing essential amenities like new electrical outlets, sinks, and emergency alarms in these repurposed spaces, the human cost remains a significant burden.

"Corridor care is the thing that causes me the greatest distress as the chief executive of the hospital and as a human being with parents and family members," Trainer admitted, his voice heavy with emotion. "I hope I never get to the stage when I walk through those corridors and don’t feel upset about it, because I’d be concerned about my loss of compassion in the face of that. It is a horrible thing to see. It isn’t acceptable to keep someone waiting in a corridor overnight on a trolley."
In a desperate plea to address the chronic overcrowding, Trainer has formally requested £35 million from the government to fund the construction of a new, state-of-the-art emergency department at Queen’s Hospital. This initiative aims to alleviate the immediate pressure and provide a more dignified and effective environment for emergency care.
The Royal College of Nursing has echoed the alarm, characterizing corridor care as a practice that has become "entrenched" across numerous hospitals throughout England. When questioned whether this descriptor accurately reflects the situation within his trust, Trainer expressed a degree of caution. "It’s difficult because it implies almost that we’re starting to accept it and we’re not," he stated. "Our third winter of corridor care is a horrible place to be in."
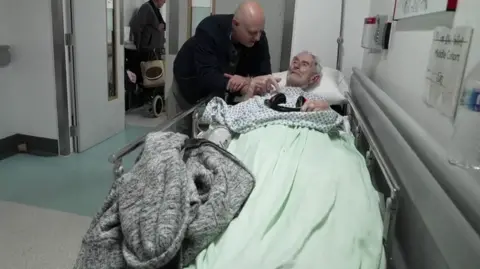
Despite the overwhelming circumstances, Trainer highlighted the unwavering dedication of his staff. "The staff come in to work around the clock to care for patients in the most dignified and respectful way they can," he emphasized. "I know from the messages I get from patients and their families they recognise the efforts the staff are putting in."
The human impact of this crisis was powerfully illustrated by the story of Cliff Mitchell, who was at Queen’s Hospital accompanying his elderly father, Roy. Roy had been on a trolley in the corridor since 6:00 PM the previous evening, a gruelling 19-hour wait before his treatment concluded. As Roy prepared to leave, Cliff described the scene with palpable frustration. "There’s people everywhere, it looks like organised chaos to me," he observed. "The staff shouldn’t be working in these conditions, patients shouldn’t be treated like this in corridors. I couldn’t even stand next to my father because there’s no space… I’m sure everyone is struggling with their loved ones. People shouldn’t be on the corridor. They should be on a ward."
Ruth Green, director of nursing in the emergency department, shared the sentiment of exasperation. "Every year I think it can’t get any worse, but this has been really, really hard," she said. "Lots of patients, long waits to be seen and a long time waiting in the emergency department. Just very, very hard for patients, relatives and staff."

The strain on the hospital extends beyond the emergency department. Queen’s Hospital’s maternity unit is one of the busiest in the country, with approximately 7,000 babies born there annually, averaging around 600 births per month. Despite its high volume, the unit, staffed by 400 midwives, received a ‘good’ rating from the Care Quality Commission in December. The latest arrival, a healthy baby boy named Landon, had been born just hours before the BBC’s visit.
New parents Holly Chilvers and Sonny Butler, experiencing the arrival of their first child, spoke of their positive experience. "I was like ‘I’m sorry I have to get him out’ and boom, 14 minutes and he was out, first baby," Holly recounted, detailing the swift birth. "It’s been absolutely fine, perfect," Sonny added. "It was a shock, definitely, when he first came out. I was struggling to hold him but the lady showed me how to do it."
Kathryn Tompsett, head of the maternity unit, acknowledged the operational challenges, stating that the service has been continuously exploring ways to deliver care "in the most efficient way" amidst ongoing NHS budget constraints. She believes that efficiency often translates into the "best care for women and their families."
Meanwhile, at the trust’s sister hospital in Ilford, King George Hospital, a different strategy is being implemented to alleviate pressure: the Elective Surgical Hub. This dedicated unit comprises nine operating theatres exclusively for planned operations, aiming to shield them from the disruptions often caused by emergency cases. Last year, the hub successfully facilitated over 10,000 planned surgeries, contributing significantly to the reduction of waiting lists.
Stuart Ayris, a former nurse awaiting knee replacement surgery, expressed his satisfaction with the efficiency of the process. "I’ve been playing cricket for the last 12 years. I’ve got a terrible batting average, so I hope that improves," he quipped, anticipating the positive impact of his surgery.
The surgical procedure was spearheaded by orthopaedic consultant Sivakumar Shankar, who utilized a robotic surgical system, one of only a handful available in the capital. "It helps us to decide what the right implant should be based on detailed imaging of the patient," Dr. Shankar explained, highlighting the precision offered by the technology. "I tell the robot what to do and then it does it. It helps us get the operation even more accurate."

As the surgical team meticulously prepared the bone for the implant, the advanced technology offered a glimpse of innovation and progress within a healthcare system facing immense pressure. While some immediate challenges at Queen’s and King George Hospitals are being addressed, more systemic issues, such as the persistent reliance on corridor care, remain subjects of ongoing effort and development.
Matthew Trainer reiterated his appeal for the £35 million needed for a new emergency department at Queen’s Hospital, recognizing its potential to alleviate immediate pressures. However, he underscored a deeper, more complex challenge: the fundamental need to develop strategies that reduce the overall number of people requiring hospital admission in the first place. This involves a multi-faceted approach, encompassing preventative healthcare, enhanced community support, and more integrated primary care services to keep people healthier and out of hospital corridors.








