General practitioners (GPs) across England are set to receive an annual bonus of £3,000 as part of a new government initiative designed to encourage and maximise the prescription of weight loss drugs to eligible patients. This financial incentive will be integrated into the GP contract starting in April, signalling a significant shift in the NHS’s approach to tackling obesity. Alongside the bonus for prescribing, GPs will also be eligible for additional funding, estimated at approximately £1,000 per year, for successfully referring patients to structured weight loss programmes. Ministers have articulated that this policy is crucial to ensuring that individuals who stand to benefit most from weight management support can readily access it through primary care.
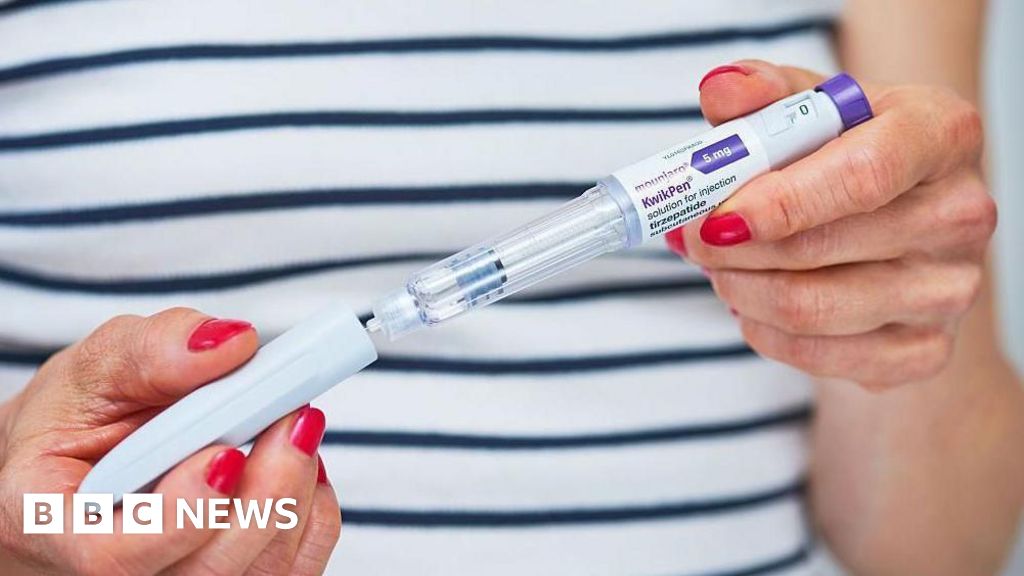
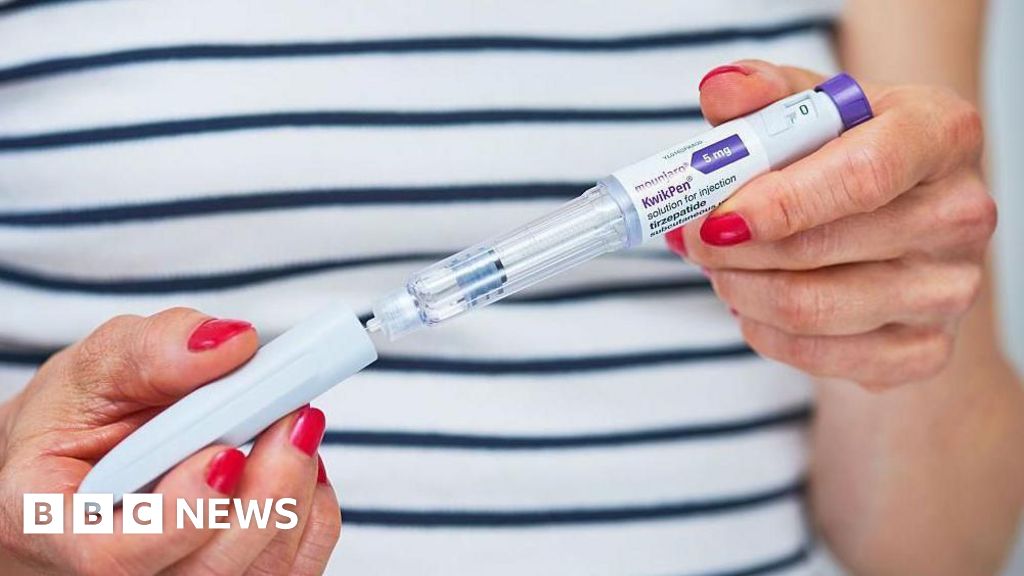
However, this proactive measure has been met with a degree of scepticism from obesity experts. They have voiced concerns that the scheme’s overall impact may be limited due to the ongoing stringent restrictions on the availability of these medications within the NHS, arguing that the incentive payments do not address the fundamental issue of widening eligibility criteria. The current financial incentive is specifically tied to the prescription of Mounjaro, a GLP-1 receptor agonist that has shown significant efficacy in weight management. It is noteworthy that another prominent new-generation weight loss drug, Wegovy, is not prescribed by GPs. Instead, its administration is managed by specialist NHS weight loss services, a distinction that may affect the reach and integration of this new incentive scheme.
The landscape of weight loss medication is rapidly evolving. Currently, it is estimated that over one million individuals in the UK are utilising injectable weight loss drugs. A striking majority, nine out of ten, are funding these treatments through private means, highlighting a significant disparity in access based on financial capacity. Health Secretary Wes Streeting has championed the new policy, asserting that "Weight loss drugs can be a real game changer for those who need them. I’m determined that access should be based on need, not ability to pay." He further elaborated on the risks associated with the current situation, stating, "Outside the NHS, we’ve seen those who can spare the cash buying privately, and the proliferation of rogue prescribers peddling dangerous unlicensed drugs that are putting patients at risk." Streeting’s vision for the policy is to "bring this modern medicine to the many, not just the few, and help shift the focus of the NHS from treatment to prevention."
Financial incentives are not new to the GP contract; they have historically been employed to drive improvements in various areas of patient care. Past incentives have been linked to enhancing dementia care, boosting vaccination rates, and promoting the prescription of statins to mitigate the risk of heart disease. This initiative marks the first instance where weight loss drugs have been explicitly incorporated into the contract, with the £3,000 bonus available to GPs who achieve the maximum prescription rate for eligible patients using Mounjaro.
The rollout of Mounjaro by GPs commenced within the current financial year, with initial access strictly limited to individuals who are severely obese, defined by a Body Mass Index (BMI) exceeding 40, and who also have specific co-existing health conditions. Looking ahead, the eligibility criteria are set to be broadened in the following year, extending to individuals with a BMI of 35 and above, alongside the existing requirement of certain health conditions. Projections indicate that by 2028, the NHS aims to have 220,000 patients receiving Mounjaro. It is important to note that eligibility thresholds are further adjusted for certain ethnic groups, reflecting a nuanced approach to addressing health disparities.
Despite these policy advancements, the practical implementation of Mounjaro prescriptions by GPs has reportedly been inconsistent. Reports suggest a patchy rollout, with not all GPs prescribing the medication at the anticipated levels. Katharine Jenner, director of the Obesity Health Alliance, acknowledged the incentive payments as a "welcome step." However, she cautioned that "This doesn’t mean weight loss drugs will suddenly be available to everyone who wants them." Jenner reiterated that "NHS access will remain very limited and focused on those with the greatest clinical need, and these treatments are most effective when combined with sustained support." She also stressed the need for a broader strategy, stating, "If we’re serious about moving from sickness to prevention, expanded treatment must go alongside stronger action to improve the food environment and prevent obesity in the first place."
Dr. Katie Bramall, representing the British Medical Association, expressed a more critical perspective, noting, "While the headlines promise much, in reality there will be no change to NHS England’s eligibility criteria for patients to access injectable weight-loss medication on the NHS." She further argued that "These proposals will do nothing over the next year to address the divide between those able to pay and those left waiting unable to afford private self-funded treatments." Echoing concerns about the practical implications for GPs, Prof. Victoria Tzortziou Brown of the Royal College of GPs stated, "GPs do not withhold treatment or prescribe based on financial incentives. Decisions are guided by clinical judgement and what is safest and most appropriate for individual patients." She also raised a pertinent point about workload, suggesting that "Widening the roll-out of these medications in general practice could end up increasing workload in a way that may not be sustainable and risk raising unrealistic expectations among patients who may not be eligible or for whom these medicines are not suitable."
The introduction of these financial incentives underscores the government’s commitment to addressing the growing obesity crisis in England. By directly remunerating GPs for prescribing weight loss drugs and referring patients to support programmes, the NHS is attempting to overcome potential barriers to uptake and ensure that evidence-based treatments reach those who need them most. The policy aims to reframe the narrative around obesity, moving from a purely treatment-focused model to one that emphasises prevention and early intervention. The hope is that by making these advanced medications more accessible within primary care, the NHS can achieve better health outcomes for a larger segment of the population, thereby reducing the long-term burden of obesity-related illnesses.
The strategic inclusion of Mounjaro in this incentive scheme is significant. As a potent GLP-1 receptor agonist, it offers a substantial benefit in terms of weight loss for many patients. The fact that it is now being managed within general practice, supported by these financial incentives, represents a decentralisation of care that could potentially improve convenience and continuity for patients. However, the effectiveness of this policy will ultimately hinge on how well the eligibility criteria align with the broader public health goals and how effectively the incentives are implemented to encourage, rather than coerce, clinical practice.
The dual approach of incentivising prescription and referral to weight loss programmes is designed to promote a holistic management of obesity. Weight loss drugs, while powerful tools, are most effective when integrated into a comprehensive care plan that includes lifestyle modifications, dietary advice, and behavioural support. The additional £1,000 per year for referrals signals an understanding of this crucial interplay between medication and behavioural interventions. This integrated approach is essential for achieving sustainable weight loss and improving overall health and well-being for patients.
The concerns raised by obesity experts and medical bodies regarding the limitations of NHS access and the potential for increased workload are valid and warrant careful consideration. While the incentives are a positive step, they do not, in themselves, solve the fundamental challenges of funding, resource allocation, and equitable access to healthcare. The debate highlights the complex interplay between financial incentives, clinical autonomy, and the broader societal efforts required to combat obesity effectively. The government’s commitment to expanding eligibility and increasing the number of patients on Mounjaro by 2028 suggests a long-term vision, but the immediate impact of this incentive scheme will be closely scrutinised by healthcare professionals and patient advocacy groups alike. The success of this policy will be measured not just by the number of prescriptions issued, but by the tangible improvements in patient health and the overall reduction in the prevalence of obesity-related diseases. The ultimate goal is to ensure that these groundbreaking weight loss medications serve as a catalyst for a healthier future, benefiting a wide spectrum of the population and shifting the paradigm of chronic disease management in the NHS.