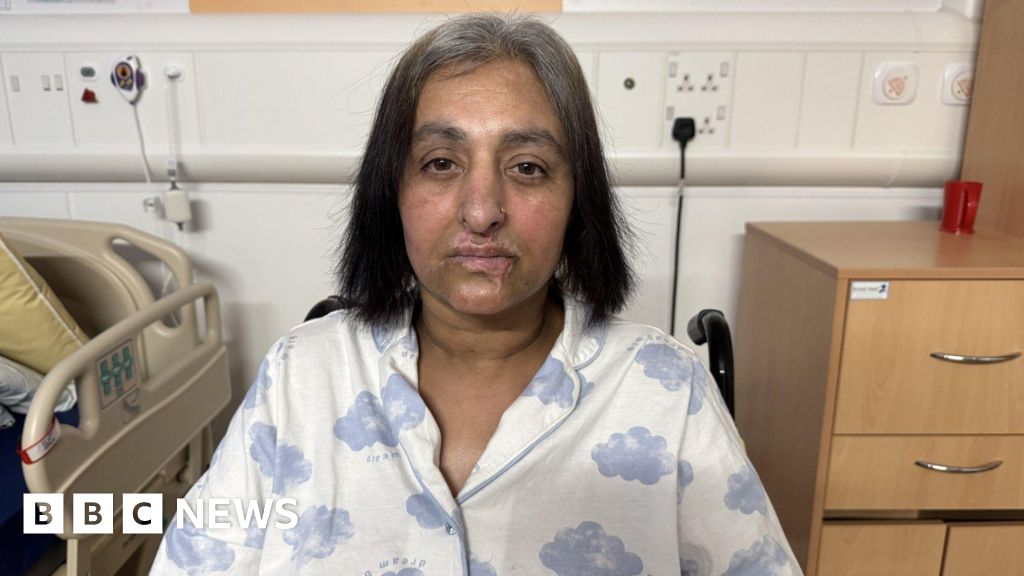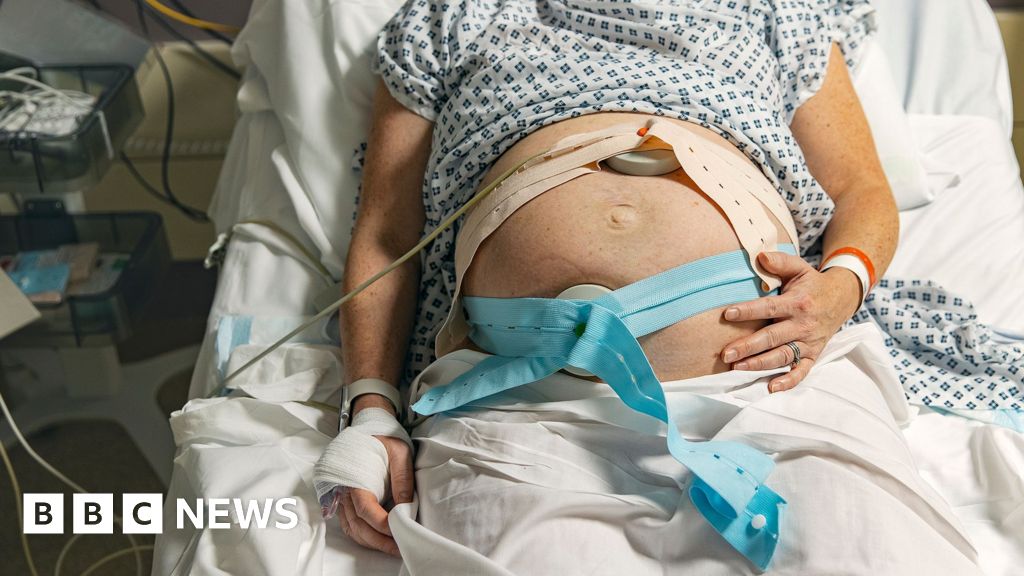
Maternity services across England are fundamentally failing "too many" families, with critical issues identified at "every stage" of the maternity journey, according to a damning interim report. The comprehensive review, spearheaded by Baroness Amos, a prominent figure in social justice, has pinpointed racism, systemic staffing shortages, and a pervasive lack of accountability as six key contributing factors to the widespread shortcomings. The investigation has already gathered a staggering amount of evidence, with over 8,000 individuals submitting their testimonies. Baroness Amos has personally engaged with more than 400 families who have experienced either trauma or exceptional care, painting a stark and often heartbreaking picture of the current state of NHS maternity provision.
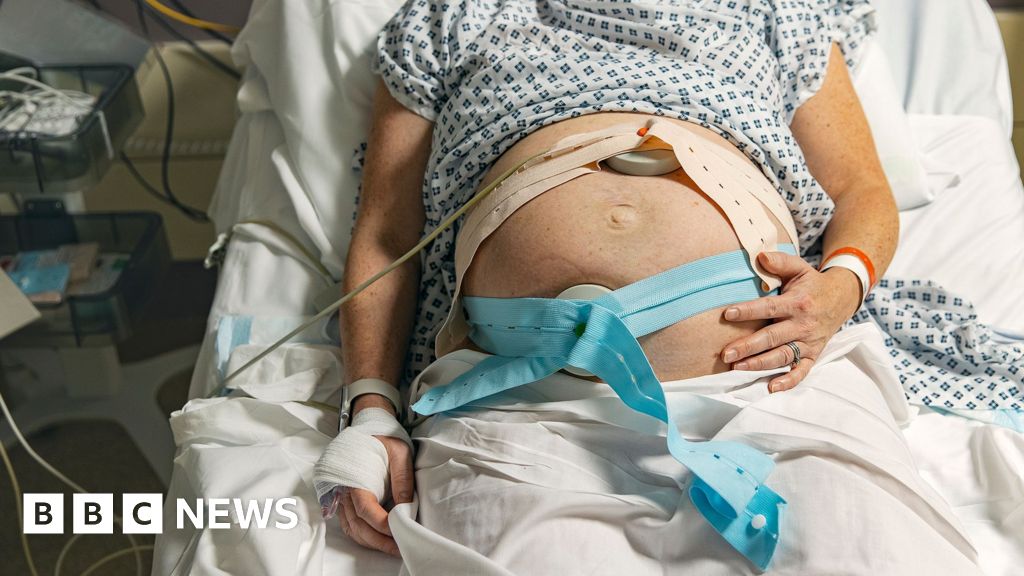
In response to these alarming findings, Health Secretary Wes Streeting has publicly pledged to implement the final recommendations of the report, which are anticipated in April. Baroness Amos, speaking candidly to BBC Breakfast, articulated the deeply inconsistent nature of care she has encountered. "I have seen bad, poor, good and excellent care co-existing side by side," she stated. "Families have described to me good experiences, terrible experiences. It is patchy, it is inconsistent and what this investigation is about, is trying to find out the things that move us from poor and bad to good and excellent." She emphatically confirmed the existence of safe and good care, citing examples she has witnessed. However, she equally stressed the overwhelming prevalence of poor care. "What I have heard from families it is so traumatic and distressing. I have seen Trusts that have changed their practices as a result of what has happened in those trusts. It is a very mixed picture. It is not consistent."
The interim report meticulously details six core areas of concern, with specific attention drawn to the insidious role of racism within maternity settings. This systemic issue disproportionately affects Black, Asian, and Minority Ethnic women, exacerbating existing inequalities and leading to poorer outcomes. The report also highlights the critical impact of inadequate staffing levels, which places immense pressure on healthcare professionals, compromises patient safety, and contributes to a breakdown in effective communication and teamwork. Furthermore, the review identifies a significant deficit in robust accountability mechanisms, leaving families without recourse and failing to drive necessary improvements within underperforming NHS Trusts.
Baroness Amos’s statement underscored the gravity of the situation: "It is clear from the meetings and conversations I have had with hundreds of women, families and staff members across the country, that maternity and neonatal services in England are failing too many women, babies, families and staff." This sentiment resonates deeply with countless families who have endured harrowing experiences.
The systemic failures within NHS maternity services are not a new revelation. For over a decade, the BBC has been documenting the accounts of bereaved and harmed families who have suffered due to inadequate care at numerous NHS Trusts across England, including the widely publicised cases at Morecambe Bay, Shrewsbury & Telford, East Kent, Nottingham, and Leeds. This extensive body of evidence, painstakingly gathered by the BBC, paints a consistent and deeply concerning picture of ongoing failings in maternity provision.

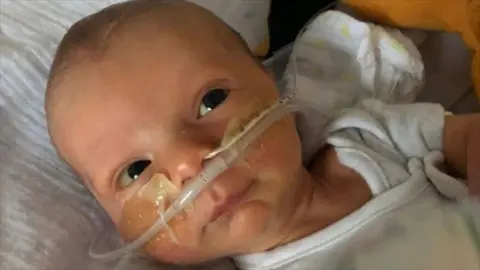
One such tragic case is that of Orlando Davis, who died at just 14 days old in September 2021. Staff at Worthing Hospital in Sussex failed to recognise that his mother had developed hyponatremia, a dangerously low level of sodium in the blood, during labour. A subsequent inquest concluded that neglect was a contributing factor to the infant’s death. Orlando’s mother, Robyn, poignantly stated that "not listening to my concerns is the main reason we’re sat here without our son." Her husband, Jonathan, believes a deeply ingrained "cultural" problem exists within maternity services, where some midwives operate under the assumption that their professional expertise supersedes the individual experiences and instincts of the mother. He argues that "the only one that truly knows what’s going on in that individual’s body is the mother."
The Davis family is actively involved with the campaign group "Truth for Our Babies," which is advocating for an independent investigation into maternity services at the University Hospitals Sussex NHS Trust. Their fight for justice highlights the broader call for systemic change. Earlier this month, a joint investigation by BBC News and the New Statesman revealed that at least 55 babies over a five-year period might have survived if they had received better care within the trust.

Despite the thoroughness of the Amos review, the Davis family, like many others, express concerns that it may not delve deeply enough to effect the radical transformation required. They are calling for a statutory inquiry, which carries greater legal weight and investigative powers. "It’s not going deep enough… it’s not just what’s happening at these hospitals. It’s the regulators as well," Robyn stated, pointing out that the regulatory bodies themselves are not under review by Baroness Amos. Jonathan added, "As families, we have received lacklustre care… We [therefore] deserve the gold standard of accountability – and progressing a rushed, high-level review, instead of a statutory inquiry, is not receiving the gold standard. Future mothers and future children may not suffer the same irreversible fate that we have if a [properly] conducted inquiry happens."
Michelle Welsh, a Labour MP and a vocal advocate for maternity safety, has voiced concerns that the Amos review might become ineffective without decisive governmental action. She is urging the government to implement substantial policy changes, including the establishment of a dedicated maternity commissioner to oversee and drive improvements in care standards. "This inquiry must result in some big, bold policies with regards to maternity services, that really says that as a government we want to improve maternity services, we want to invest in it, and we will secure the truth and accountability for families," she asserted.
When the review was announced last June, Wes Streeting also committed to chairing a maternity taskforce early this year to expedite improvements. However, it has emerged this week that this crucial taskforce has not yet been formally established. The Department for Health and Social Care has stated that membership will be announced "shortly." Welsh emphasised the urgency of this matter, stating, "It is important that the taskforce is established as soon as possible… because without it we don’t have that driving force [and] those big, bold policies." The delay in establishing this taskforce raises further questions about the government’s commitment to swift and meaningful action in addressing the critical failings within England’s maternity services.