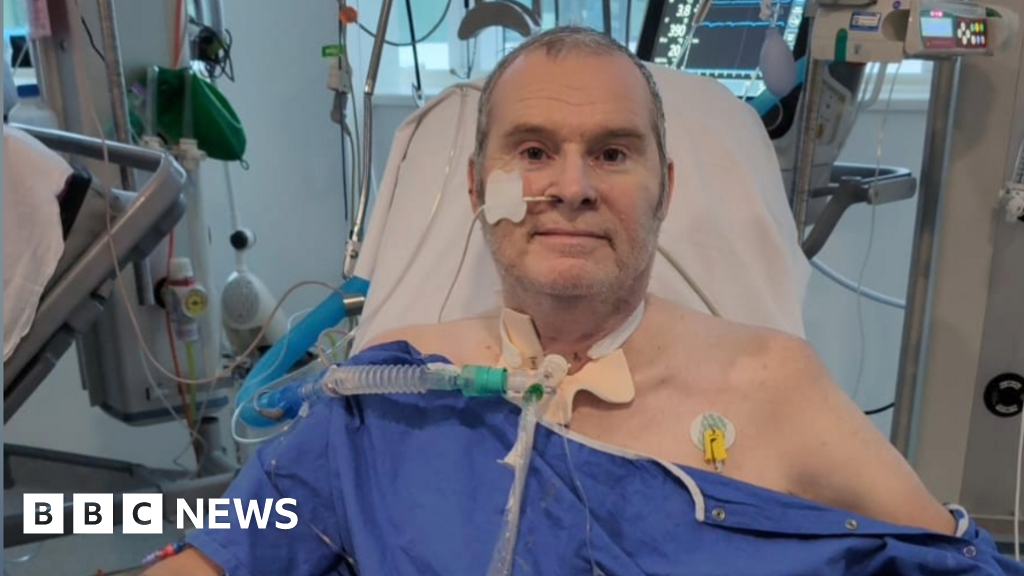
For Matthew Smith, each morning began with a quiet hope, a fervent wish for the phone call that would signify a second chance at life. Diagnosed with a terminal lung condition in 2023, he found himself navigating the agonizing limbo of the organ transplant waiting list for nearly a year, the shadow of his illness a constant companion. "From when you first wake up, you think, is today going to be the day we get that call?" he recounted, the weight of those words still palpable. His wife, Nicola, from Wednesbury, echoed his sentiment, admitting to waking through the night, her phone clutched tightly, terrified of missing that life-altering notification. "I would wake up through the night just to double check my phone that I haven’t slept through a phone call," she shared.
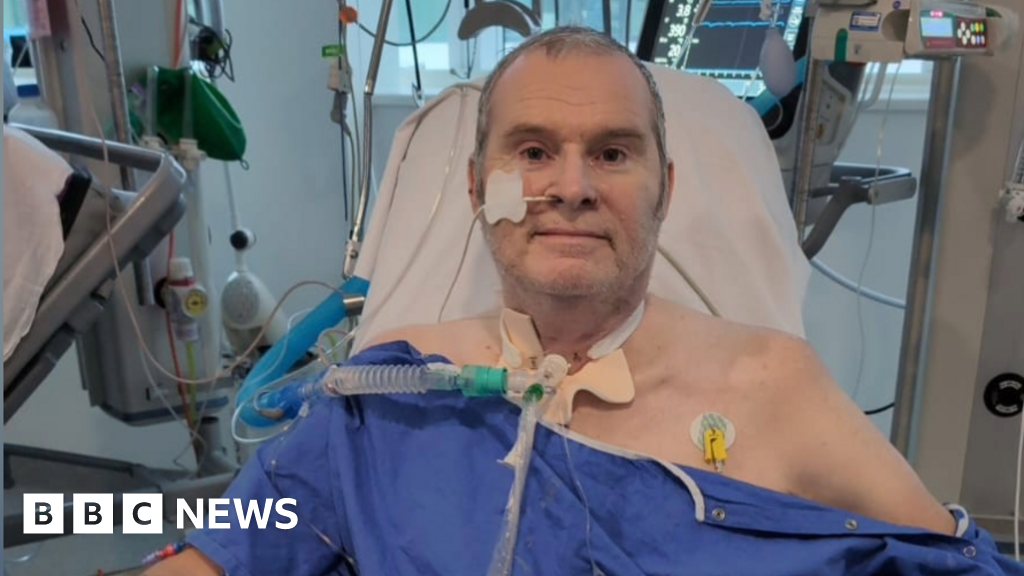
The call, when it finally arrived after a grueling ten months, marked not an end, but a new beginning. Yet, Matthew’s story is a stark reminder of a growing crisis: over 8,000 people in the UK, a record number, are currently awaiting organ donations. While the demand for life-saving transplants has surged to unprecedented levels, the rate of donor consent has plateaued, leaving a widening chasm between those in desperate need and the availability of organs. Increasingly, families are opting against allowing their deceased loved ones’ organs to offer hope to others, a decision that directly translates into longer, more perilous waits for individuals like Matthew and the 500 others in the West Midlands facing similar uncertainties.
The introduction of an "opt-out" organ donation system in England in 2020, following Wales’ implementation five years prior, was hailed as a landmark reform. Under this system, consent for organ donation is presumed for all adults unless they explicitly register their objection. In 2018, Theresa May’s government projected that this shift could save up to 700 lives annually. However, a significant loophole remains: grieving families retain the power to override a deceased individual’s wishes, even if they were registered organ donors. This familial veto has become a significant barrier, contributing to the stagnation in donation rates.
The reasons cited by families for blocking donations are multifaceted and often deeply personal. They range from a lack of clarity regarding the deceased’s wishes, a perception that the donation process is too time-consuming during a period of intense grief, a reluctance for further surgical intervention on the body, to deeply held religious or cultural beliefs that may not align with organ donation. These deeply human considerations, while understandable, have a direct and often tragic impact on the waiting list.
Christine Cox MBE, a tireless advocate for organ donation for over three decades, understands this struggle intimately. Her journey began in 1989 after the death of her brother, Peter, who succumbed to a brain tumour at the young age of 24. While Peter’s illness meant his organs could not be donated to save him, his final wish was to benefit others. "It was his final wish that his life should benefit others and indeed 17 people benefitted from him donating all of his organs when he died," she explained, her voice filled with the enduring pride of her brother’s selfless act. "He did say it was our duty to ensure that as many organs as possible could benefit others."
In the aftermath of Peter’s death, Christine and her parents discovered a critical gap: there was no formalized system for registering organ donation intentions. This realization ignited a relentless campaign that culminated in the establishment of the organ donor register in 1994. Prior to this, organ donation was entirely reliant on individuals carrying physical organ donor cards, a system fraught with practical challenges. "People didn’t always carry the donor card on them in their pockets and handbags and the nurses and doctors didn’t have time to look through. So there was a problem," Cox recalled, highlighting the logistical hurdles that often prevented timely donations.
While Cox was initially jubilant about the introduction of the opt-out system, she soon recognized its "fatal flaw" – the persistent ability of next of kin to override a donor’s explicit wishes. Her enduring message, honed through years of advocacy, centers on the crucial importance of open communication. "I implore everybody not just to make their wishes known but to talk to their friends and their family and also find out what their friends and family want," she urged. "It possibly will never happen however everyone needs to know what your wishes are." This sentiment is a cornerstone of the NHS’s "Hope Takes Flight" campaign, which endeavors to encourage families to engage in these vital conversations before it is too late.

Harpreet Matharu, an organ donation specialist nurse for the NHS, corroborates Cox’s emphasis on communication. "What we’ve always said is talk to your loved one, make a decision and sign on the register, because we know when a patient has opted in and had those conversations, consent is much higher in those circumstances," she stated. Matharu also addresses common anxieties surrounding the donation process, particularly for those who may feel squeamish about the concept. She emphasizes that the process is conducted with the utmost respect, and all religious and cultural needs are meticulously catered for. "When you donate, you are looked after with the upmost respect in hospitals and all your religious and cultural needs are still catered for," she assured.
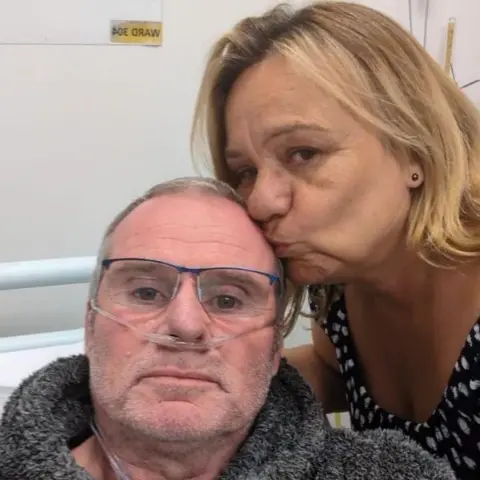
For Matthew and Nicola Smith, the transplant was more than a medical procedure; it was a profound rebirth. Nicola described the day of the surgery as "a very long day," admitting to tears from the moment Matthew was taken in until his return. "It’s the start of a new beginning. It’s a new life," she said, her voice brimming with emotion. "He can do so much more now, he can take part in things. It just feels like his life’s just beginning again now." Their shared hope for the future includes renewing their vows on their 30th wedding anniversary this year, a testament to their enduring love and Matthew’s renewed vitality.

Nicola’s heartfelt plea serves as a powerful call to action: "You’re giving somebody the chance of a new future, to live a good, long life. To make memories." This sentiment underscores the immense power of organ donation to transcend individual lives and create a ripple effect of hope, offering not just a physical gift, but the invaluable opportunity for continued existence and the creation of cherished memories. The challenge of increasing organ donation rates is a societal one, requiring a shift from passive consent to active, open conversations that honor individual wishes and ultimately save lives.







