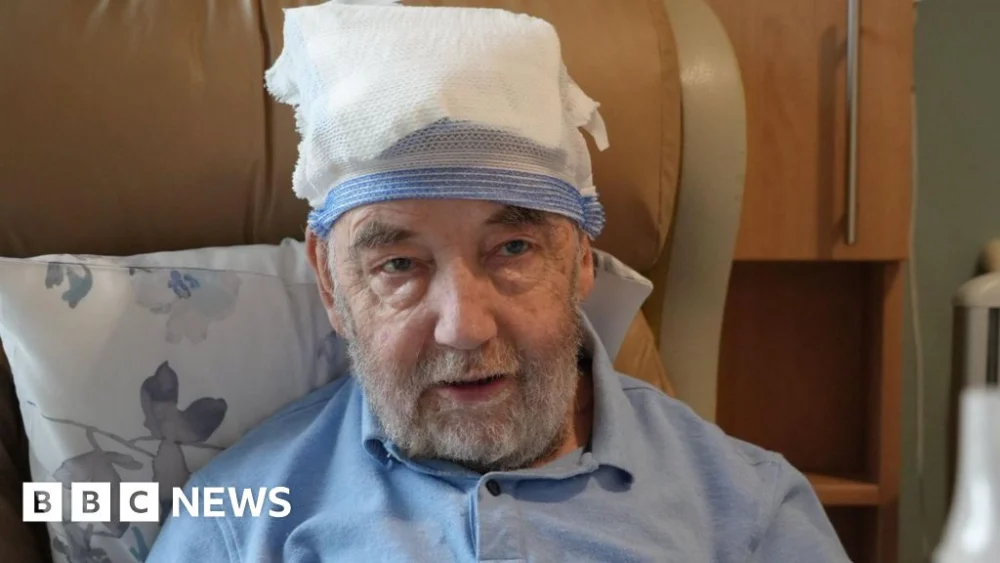
Paul Thomas, a 58-year-old from Flint, found solace and relief at St Kentigern Hospice in St Asaph after struggling alone at home, describing the end-of-life care he received as transformative in managing his pain and anxieties. "I think everybody worries when they come to the last stages, no-one knows what to expect, but these people are wonderful at relaxing you and they help you an awful lot," he shared, highlighting the profound impact of hospice care on his well-being. However, this vital support system is facing an existential threat, with Hospice UK warning that the current funding model is unsustainable and could lead to a reduction in services for those nearing the end of their lives.
The stark reality of the financial strain on Welsh hospices is underscored by the fact that nine out of the fourteen hospices in Wales anticipate facing a financial deficit in the 2025-26 financial year. Compounding this crisis, one hospice has already closed its doors permanently, and another has been forced to temporarily shut down its services due to escalating running costs and persistent funding difficulties. These closures and potential reductions represent a significant blow to palliative care provision in Wales, leaving vulnerable individuals and their families with fewer options during their most critical times.
Paul’s experience vividly illustrates the compassionate and personalized care that hospices provide, a stark contrast to the often overwhelming environment of a hospital. Upon his arrival at St Kentigern, he was immediately made comfortable, his belongings were unpacked, and his dietary preferences were catered to. "They did a really nice chicken curry and Eton mess, and I slept for about 16 hours. I was shattered," he recalled, emphasizing the attentive and individualised approach. He further elaborated on the emotional benefits, stating, "It brings me a lot more comfort, a lot more serenity and they discuss things with you in a more sedate and gentle way." The ability to receive friends together in a peaceful setting, a luxury often unattainable in a hospital, was also a significant comfort. "It was quite quiet and peaceful. A bit of laughter, but not too much because it’s not the time to laugh now is it?" he reflected. The staff’s dedication to his comfort and safety was paramount: "I feel comfortable and safe, and at this period it’s very important."
Across Wales, approximately 20,000 adults and children affected by terminal illnesses rely on hospice services annually. While Welsh hospices collectively offer 95 inpatient beds, the ongoing financial and staffing challenges mean that some of these beds may not be operational. Furthermore, a significant portion of hospice care, around 60%, is delivered within the community, providing essential support in patients’ own homes.
Hospices Cymru, the charity representing hospices in Wales, has issued an urgent plea to the Welsh government and health leaders to safeguard these crucial services by overhauling the existing funding model. Liz Booyse, chair of Hospices Cymru, highlighted the precarious financial situation, noting that, on average, only 30% of hospice funding comes from the Welsh government and the NHS, while the remaining 70% is generated through charitable donations. This heavy reliance on donations makes hospices particularly vulnerable to economic downturns and fluctuating public generosity. "Hospices will be making decisions right now as to the future of the services they can offer… they’re making difficult decisions," she stated, underscoring the immediate and critical nature of the funding crisis. Moreover, the demand for palliative and end-of-life care is projected to increase significantly, with an estimated 25% rise in need over the next 25 years, further exacerbating the strain on already stretched resources.
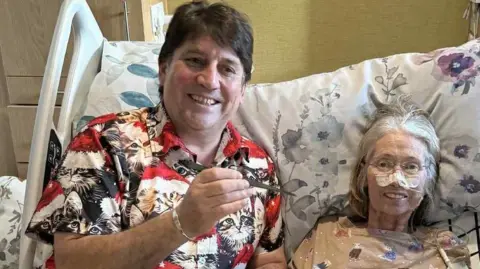
The personal testimonies from families underscore the unique and invaluable nature of hospice care. John Owen shared the poignant experience of his wife, Rowena, who was diagnosed with a rare form of cancer in 2024. Describing Rowena as "an amazing person" who "loved life and was such a kind, caring and compassionate person," John expressed his wish for her to receive care at a hospice. "We wanted the hospice to care for her, and then we could just care for her loving needs and that’s exactly what happened," he said. The hospice staff went above and beyond to fulfil their wishes in Rowena’s final days, even facilitating a visit from their beloved cats, allowing Rowena to experience the comfort of stroking them. "We brought [our] two cats in and she was able to give them a stroke, which was amazing," John recounted. The installation of a "cuddle bed" was another pivotal element of their experience, enabling John to stay with Rowena 24/7 for 12 days. "It was such a comfort to both of us because it meant I could stay with Rowena 24/7 – which I did for 12 days. It was incredibly sad and hard work but they made it as best as it possibly could be for us," he shared. Moved by the experience, John has now embarked on fundraising for another cuddle bed for the hospice, hoping to extend this vital comfort to other families. He echoed Paul’s sentiment, agreeing that hospice care offered a calmer environment than hospitals and lamented the underfunding: "The fact that they’re not funded enough is really sad because they are vital."
The operational impact of the funding crisis is already evident. In the past year, Shalom House Hospice in Pembrokeshire has ceased operations, and a four-bed inpatient unit at St David’s Hospice in Holyhead has been temporarily closed due to the prohibitive increase in running costs and funding shortfalls. These closures represent a significant loss of specialized end-of-life care capacity in their respective regions.
The Welsh government has acknowledged the crucial role of hospices in end-of-life care and has stated that it is actively engaging with them to understand their challenges better. A spokesperson confirmed that investment in hospices has seen a substantial increase during the current Senedd term, with an additional £5.2 million allocated annually and over £9.5 million provided in one-off grants. These funds are intended to help the sector manage rising costs and sustain essential services. Furthermore, the government is developing a new hospice commissioning approach aimed at ensuring equitable access, long-term financial stability, and the delivery of high-quality care across Wales.
Political parties have also weighed in on the issue. Plaid Cymru has indicated its commitment to exploring ways to enhance the sector’s financial sustainability and plans to implement comprehensive governance reforms within the NHS to improve end-of-life care provision. The Welsh Conservatives have pledged to introduce a new sustainable funding model and provide an additional £40 million over the next Senedd term, arguing that substantial tax increases have forced the sector into making difficult choices. The Liberal Democrats are calling for the UK and Welsh governments to reverse the National Insurance increase affecting hospices, establish a sustainable funding settlement, ensure pay parity for hospice staff with their NHS counterparts, and implement long-term contracts for hospice services throughout Wales. Reform UK and the Welsh Green Party have been approached for comment.
The continued underfunding of Welsh hospice services poses a significant risk to the availability and quality of end-of-life care, impacting thousands of individuals and their families at a critical juncture in their lives. The urgent need for a robust and sustainable funding model is paramount to ensure that these vital institutions can continue their compassionate work.






