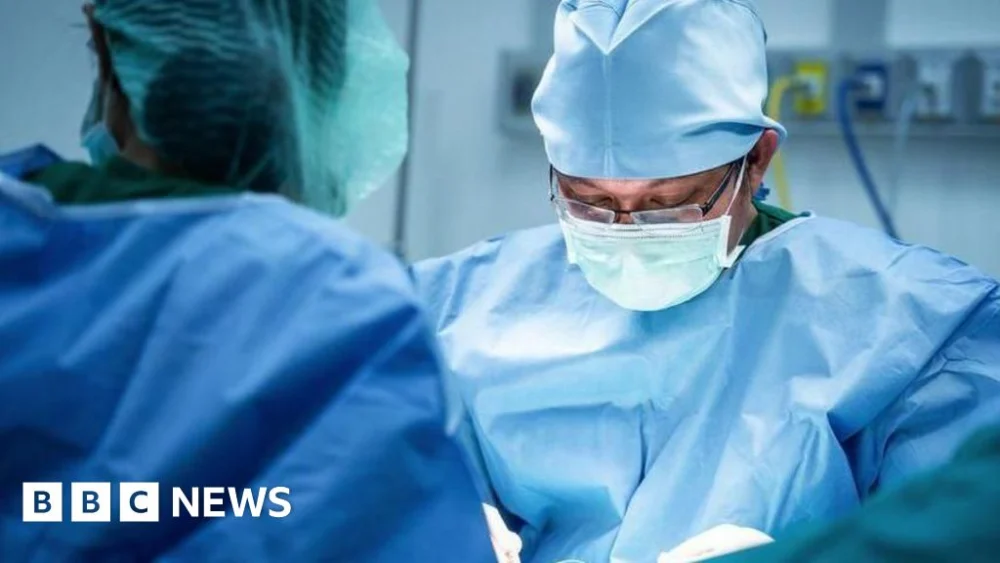
The government’s commitment to reducing waiting times, particularly for procedures like knee and hip replacements, has been a central pledge. However, the reality on the ground suggests that the ambitious targets set out a year ago are proving difficult to achieve for many institutions. The reasons cited by the struggling hospitals are a complex web of interconnected challenges, including critical staffing shortages, the disruptive impact of industrial action by doctors, and the persistent issues with outdated or malfunctioning IT systems. These factors combine to create a perfect storm, exacerbating existing pressures and pushing waiting lists further into the future.
One poignant example of the human cost of these delays is Mary Waterhouse, a 72-year-old from Blackpool. Diagnosed with severe arthritis, Mary has been navigating the healthcare system since 2022. After initial steroid injections, her condition worsened, leading to her re-admission to the waiting list in late 2024. The subsequent eight-month wait for an assessment was a period of intense suffering, during which her health deteriorated to such an extent that she was informed she would require hip and knee replacements on both sides. Faced with the prospect of multiple complex surgeries and an uncertain recovery, Mary made the heartbreaking decision to forgo treatment, choosing instead to "live with the pain."
"I had long waits at every stage since first being referred," Mary recounted, her voice tinged with weariness. "It’s like being in a never-ending queue." The impact on her daily life has been profound. She now relies on a mobility scooter for anything beyond short distances and uses crutches to navigate even the most basic movements. "If I had received quicker treatment, things may have been better," she lamented, a sentiment echoed by countless others in similar predicaments.
Deborah Alsina, from Arthritis UK, highlighted Mary’s experience as a "typical" case, illustrating the widespread difficulties faced by individuals living with arthritis. She stressed the "life-changing" potential of timely treatment, but lamented the "inequitable access to care" that many patients are experiencing. Blackpool Hospitals NHS Trust, while unable to comment on Mary’s specific case, acknowledged the unacceptably long waits. Chief executive Maggie Oldham stated, "We know we’re not where we need to be, but we’re continuing to work hard alongside our partners to address the issues we’re facing urgently."
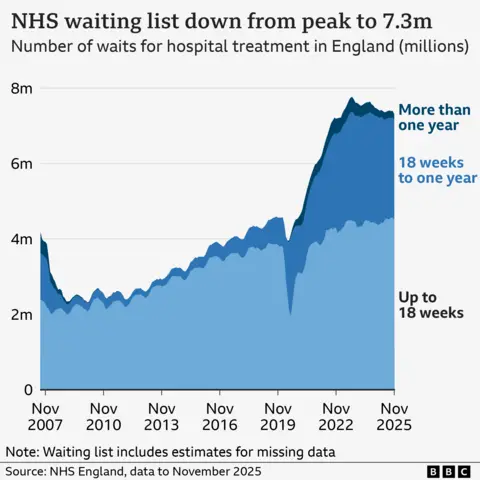
The government’s stated ambition is to return to the 18-week waiting time target for routine treatments in England by March 2029, a goal that has not been met since 2015. The target itself requires 92% of patients to be seen within this timeframe, a benchmark that now seems a distant aspiration. An interim target of 65% has been set for March 2026, a more modest but still challenging objective. When the government’s recovery plan was unveiled last January, only 59.2% of patients were waiting less than 18 weeks; this figure has since improved to 61.8%. The overall waiting list has also seen a slight reduction, falling to 7.31 million, its lowest point since February 2023.
Despite these national figures, the BBC’s analysis, which compared current performance with data from 12 months prior for all but two hospital trusts (data for Sheffield and Barking, Havering and Redbridge trusts was unavailable), reveals significant disparities at a local level. The data, reflecting performance up to November 2025, shows that the vast majority of the progress made has been concentrated in certain areas, while others have regressed.
East Cheshire NHS Trust has experienced the most substantial decline, with the percentage of patients waiting less than 18 weeks dropping from 61.2% to 51.2%. Barnsley Hospital NHS Foundation Trust saw a concerning decrease of nine percentage points, while Whittington Health NHS Trust and Epsom and St Helier University Hospitals NHS Trust both recorded falls of approximately five percentage points.
The trusts themselves attribute these declines to a confluence of factors. Epsom and St Helier, for instance, pointed to the disruptive impact of implementing a new electronic patient record system, which led to temporary service interruptions. Barnsley cited severe staff shortages and the urgent need to prioritise cancer referrals, which inevitably pushed back the scheduling of planned treatments. The ongoing industrial action by junior doctors also emerged as a significant contributor, with the frequency and impact of strikes varying considerably across different regions.

Despite these challenges, several trusts expressed optimism about future improvements. Both Barnsley and Epsom and St Helier indicated that they anticipate a reversal in the negative trend. On the positive side, 98 NHS trusts have shown improvement over the past year. However, for 17 of these, the progress has been marginal, an increase of less than one percentage point. Conversely, a handful of trusts have demonstrated remarkable turnaround stories. Five NHS trusts have achieved significant improvements, with gains ranging from nine to 10 percentage points. Notably, Shrewsbury and Telford Hospital Trust, which was previously among the poorest performers, has seen a dramatic improvement of 17 percentage points.
The 18-week pledge is specific to England, but the struggle to meet targets for hospital treatments is a pervasive issue across the entire United Kingdom. Rory Deighton, from the NHS Confederation, which represents NHS trusts, emphasised the complexity of the situation. He noted that "the NHS is not one homogenous body but is made up of hundreds of separate organisations, each with their own distinct financial and operational challenges." This inherent variability means that addressing care backlogs will inherently be more challenging in some regions than others, particularly where "entrenched challenges, such as high levels of local deprivation" exist.
Chris McCann, deputy chief executive at patient watchdog Healthwatch England, underscored the "stark differences" faced by patients depending on their geographical location. He urged those responsible for monitoring NHS trusts to pay "close attention to organisations that are not only performing poorly but actually deteriorating."
A spokesperson for the Department of Health and Social Care maintained that the government is "on the road to recovery" for the NHS, while acknowledging that "there is still more to do." They highlighted ongoing investments in services such as new surgical hubs and expanded scanning capabilities during evenings and weekends as crucial steps towards alleviating pressure. The department also affirmed that individual hospitals will be held accountable for their performance, suggesting a renewed focus on local responsibility and outcomes. The journey towards a consistently functioning and accessible NHS remains a formidable challenge, with the "never-ending queue" a stark reality for too many.






